 Athlete’s foot is caused by a fungal infection of the skin on the foot. The majority of these infections are caused by one of three types of fungi called dermatophytes. Athlete’s foot is by far the most common fungal infection of the skin. The infection can be either acute or chronic. The recurrent form of the disease is often associated with fungal toenails or Onychomycosis.
Athlete’s foot is caused by a fungal infection of the skin on the foot. The majority of these infections are caused by one of three types of fungi called dermatophytes. Athlete’s foot is by far the most common fungal infection of the skin. The infection can be either acute or chronic. The recurrent form of the disease is often associated with fungal toenails or Onychomycosis.
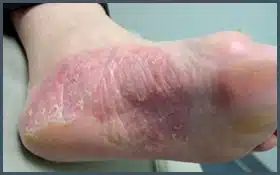
The acute form of the infection most often presents with moisture, scaling between the toes with occasional small blisters and/or fissures. As the blistering breaks, the infection spreads and can involve large areas of the skin on the foot. The burning and itching that accompany the blisters may cause great discomfort that can be relieved by opening and draining the blisters or applying cool water compresses. The infection can also occur as isolated circular lesions on the bottom or top of the foot. As the skin breaks down from the fungal infection, a secondary bacterial infection can ensue.
The chronic form of athlete’s foot is a relatively non-inflammatory type of infection. It is characterized by a dull redness to the skin and pronounced scaling. It may involve the entire bottom of the foot giving a “moccasin” appearance. It generally does not itch or result in the formation of blisters. This form of the disease frequently has an associated fungal infection of the toenails.
Diagnosis
The diagnosis of tinea pedis is generally made based on the clinical presentation. A definitive diagnosis is made by taking a scraping of the skin and culturing it. It may take up to three weeks for the culture to grow the fungus. In some instances, the culture may present a false negative result because the skin scraping was inadequate. Some doctors may perform a KOH prep of a skin scraping. This is examined under a microscope and may reveal elements that can make the diagnosis.
Treatment
Treatment should be directed at controlling the fungal infection and treating any secondary bacterial infection with oral antibiotics. Soaking the feet in Epsom salts and warm water is helpful. Powders to control moisture and OTC topical antifungal medications can also be used. If these are not effective, call Family Podiatry.
